Absorption of Nutrients as You Age
There’s no doubt about it: our nutritional needs change as we age. You may have eaten 2,500 calories as an active 25-year-old, but as a sedentary 60-year-old, that’s way too much food. There’s nothing wrong with slowing down as we age, it’s a natural process, but the struggle to get all the necessary nutrients becomes harder. Unfortunately, this results in many older adults having vitamin deficiencies which lead to a whole slew of other conditions. Vitamin deficiencies affect all our organs, not in the least our eyes.
Why Absorption Changes with Age
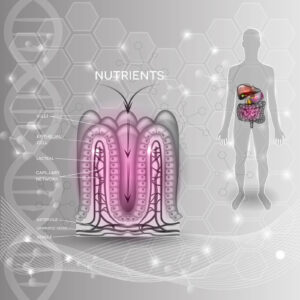
As we mentioned, our appetites tend to decrease as we get over the hill and become seniors. Elderly people are notorious for not eating enough and therefore being deficient in nutrients. Then there are the gastronomical issues that arise when we age. Different stomach and digestion conditions force us to eat less or alter our diets. For example, atrophic gastritis, GERD, and diverticulitis all affect the adult population and their food choices.
One of the most common absorption issues in adults is the lack of stomach acid. It’s been proven that stomach acid naturally decreases as we age. We need stomach acid to break down our food and help our bodies absorb the nutrients. The nutrients that are notably not absorbed when this happens are magnesium, iron, calcium, and vitamin B12.
Common Vitamin Deficiencies of Older Adults
Vitamin deficiencies are a serious issue, especially among seniors. This demographic is already eating fewer calories and living more sedentary lives. Removing vital nutrients from their diet only encourages health conditions to develop. Here’s what can happen if older adults are deficient in the nutrients commonly non-absorbed.
Magnesium Deficiency
The body naturally makes cells and free radicals. Free radicals are by-products of oxygen interacting with certain molecules. If our free radicals aren’t neutralized, they can cause severe damage to our cells, resulting in heart disease, cancer, and cataracts. We neutralize our free radicals by eating foods rich in antioxidants, like magnesium.
Older adults who are deficient in magnesium due to malabsorption see their bodies overproduce free radicals. This means they’re more likely to develop the diseases mentioned above. Our eyes are especially affected by magnesium deficiencies because free radicals wreak havoc on our eye cells. Without magnesium, we’re more likely to develop age-related macular degeneration and cataracts.
Iron Deficiency
Anemia, also known as iron deficiency, is a common condition at any age. But older adults and seniors are especially prone to developing it due to their decrease in stomach acid. Some of the most common symptoms of anemia are also, sadly, symptoms of aging. For example, fatigue, muscle weakness, low blood pressure, and lightening of the skin. Without a blood test, seniors with anemia could go untreated. Our eyes suffer greatly when we’re low in iron. Blurred vision, dizziness, and eye floaters can result from anemia.
Calcium Deficiency
We all know that calcium is the bone and teeth nutrient. Without it, our bones become brittle and we increase our risk of osteoporosis. Unfortunately, as we age, we naturally increase our risk of bone conditions. Adding a calcium deficiency to our plate will only worsen our odds. Seniors with calcium deficiencies may notice brittle nails, muscle cramps, and frequent bone fractures from seemingly harmless movements. Someone with a calcium deficiency may also notice twitching in the muscles around the eyes. There are many ways to fight a calcium deficiency, so talk to your doctor about what you can do.
Vitamin B12 Deficiency
People who are deficient in vitamin B12 can experience some strange symptoms. They might notice a smooth tongue, pale skin, nerve sensitivity, and even vision loss. The reason for the wide array of symptoms is that B12 wears many hats when it comes to helping the body. It helps make red blood cells, supports bone health, prevents anemia, and even reduces your risk of macular degeneration. Seniors who are deficient in B12 due to malabsorption will quickly notice its effects on their bodies and mental health.
What You Can Do About It
The first step to preventing malabsorption due to decreased stomach acid in aging is to live a healthy lifestyle. Be active! You should do at least 30 minutes of aerobic exercise each day. Take a brisk walk or go for a bike ride while the weather allows. Eat a nutritious diet that contains all the necessary vitamins for eye health and an aging stomach. Drink ample amounts of water each day. Living a healthy lifestyle is the front line of prevention against age-related conditions.
If you experience absorption issues as you age, as most people do, don’t worry. It’s important that you see your doctor to learn how to handle the decreased acidity in your stomach. They may prescribe you medication, but there are natural ways to increase stomach acid. For example:
- Eat fermented vegetables to fight harmful stomach bacteria.
- Drink hot water with meals, as cold water prevents stomach acid production.
- Stop eating processed and highly-refined foods that detract from stomach health.
- Try to relax when eating and avoid stress.
Sometimes our bodies develop sensitivities to certain foods when we age, which can make getting all the nutrients we should even more difficult. Things that never used to cause problems now cause heartburn. As difficult as it may be, don’t force yourself to eat these foods. You may have to get creative in finding other healthy options with the same nutritional value.
When in doubt, talk to your doctor about taking a multivitamin or supplement. This is a popular option among older adults and seniors whose appetites have naturally decreased. Taking a supplement can cover all the nutritional bases without the negative side effects of eating certain foods. It can also target important issues of concern, like your vision. You may want to consult a nutritionist or dietician to learn the best ways to take supplements when dealing with low stomach acid levels. Just remember, even though your absorption abilities change as you age, you don’t have to sacrifice getting the proper nutrient intake.



I have 2 cataracts in both eyes and a stye in the right eye also. I wear glasses to read. I am interested in rebuilding my vision.
Thanks